Blog by Matthew McKenzie aimed at unpaid carers whose cared for will soon be discharged from hospital. Here are some tips to take note of to help in smooth transistion back into the community.
To watch the video lecture nearly 30 mins, see below.
Blog by Matthew McKenzie aimed at unpaid carers whose cared for will soon be discharged from hospital. Here are some tips to take note of to help in smooth transistion back into the community.
To watch the video lecture nearly 30 mins, see below.
In this blog post, if you are involved at your local mental health NHS trust as a carer or patient. This blog will help you learn about the crucial roles of key staff in implementing the Patient Care Race Quality Framework in Mental Health Trusts.
From leadership to community engagement, discover how systematic changes can address racial disparities and promote accountability.
If you want to watch the video, this please click on the item below.
Mental health services play a crucial role in supporting individuals through challenging periods in their lives. However, despite their importance, these services have often fallen short when it comes to providing equitable care to individuals from minority backgrounds.
Continue readingWelcome to a brief update of my ethnic mental health carers forum. For this month we were joined by South West London & St George research team. The team from a training company introduced a cultural capability training program aimed at reducing race and ethnic disparities in mental health care, while Matthew presented a summary of various reports highlighting health inequalities faced by ethnic minorities in the UK. The Forum also discussed the importance of advocacy for carers, the challenges of engaging with diverse communities. A carer from South Yorkshire also discussed the potential for setting up a group to support black people in the area.
Cultural Competence Training for Trusts
The training company introduced a cultural capability training program they are developing for the South West London and St. George’s Mental Health Trust. The program is part of an ethnicity and mental health improvement project and aims to reduce race and ethnic disparities in mental health care. Representatives from the team also discussed their evidence review on cultural competence in mental health care and their use of a model of cultural competence. The training is expected to impact staff, carers, and patients by promoting culturally sensitive care plans and reducing inequalities. The team also discussed the potential to tailor the training for other trusts.
Addressing Health Inequalities and Disparities
Matthew presented a summary of various reports highlighting health inequalities and disparities faced by ethnic minorities in the UK. He emphasized the importance of these reports in supporting the Patient Care Race Equality Framework (PCRF) and other initiatives addressing health inequalities, discrimination, and racism. The reports, from organizations such as the NHS Race and Health Observatory, Public Health England, and the CQC, demonstrate that ethnic minorities face higher risks with certain health conditions, barriers to accessing services, and poorer health outcomes.
Matthew also mentioned the role of institutional racism, socioeconomic disparities, and cultural barriers in perpetuating these disparities. He concluded by emphasizing the need for systematic reforms to ensure equitable health outcomes for all.
Addressing Healthcare Disparities and Trauma
Laura from Cygnet HealthCare expressed her appreciation for Matthew’s ability to present information in an understandable and accessible manner, which she believes is not done enough. She also highlighted the importance of Matthew’s role in educating others and ensuring the right actions are taken. A carer member of the group then brought up a report from the Race Equality Foundation and Learning Disability England, which highlighted disparities in access to healthcare for ethnic minorities with learning disabilities. She shared her personal experience of a young person with a learning disability, autism, and mental health issues facing challenges during the COVID-19 pandemic. The group acknowledged the system-generated trauma faced by carers and the need for more awareness and action on these issues.
Mental Health and Learning Disability Event
In the meeting, A carer highlighted the upcoming mental health and learning disability listening event, which was previously cancelled due to lack of awareness. Others at the meeting expressed their support for the event and the importance of advocating for carers.
A representative from Surrey & Borders NHS trust who is the programme lead for carers and co-production, discussed the Trust’s co-production framework and their efforts to reach a diverse community for co-production opportunities. She also mentioned the Trust’s strategy to mirror the triangle of care. Matthew shared his experience at the Trust’s learning event and his plans to help promote the Trust’s work, particularly in relation to carer involvement.

Mental Health Event Postponement Concerns
A carer expressed surprise at the postponement of a mental health and learning disabilities listening event, which was initially scheduled for September. Another carer, who is relatively new to the Maudsley, had not been aware of the event’s postponement and was concerned about its lack of awareness. She had reached out to various individuals within the organization, including others, to discuss the event. Carers suggested that the carer should also speak to Zoe Reed or Shania, who are in charge of PCREF, to ensure the event’s success. The carer agreed to continue her efforts to promote the event and ensure its awareness.
Supporting Black Mental Health Groups
Carers discussed the potential for setting up a group to support black people in South Yorkshire, with Matthew suggesting that funding could be sought from the ICB and the charity associated with their NHS trust. A carer shared his experiences with a similar group in Peterborough, emphasizing the need for more conversation and less medication in mental health care for black people. A Carer, who is involved in setting up a group in Kent, shared her challenges due to the predominantly population in her area. Matthew also mentioned an upcoming event on the new Mental Health Act and its potential impact on carers. The team agreed to reconvene in January.
Welcome back to a brief update of another group I chair with support of London Hospitals and the carer centres of London, along with carers who want the best service of those using the NHS.
The group is called the “Carers hospital discharge toolkit meeting”. This group runs every 2 months and follows off the work the previous NHS England carer lead for London developed.
The community deserves the best care possible from the NHS and that includes carers who support those they care for using the hospitals in London and beyond. This was taken up by NHS England Carer lead for London Debbie Hustings who worked very hard to produce the toolkit linked below.
London Carers Hospital Discharge toolkit
Feeling passionate on continuing the work, Carer centres and hospital representatives came together to support me in driving this brilliant toolkit. The group has been running 2 years and developing rapidly.
Here is the update for November 2024
The meeting for November focused on the development and progress of various resources aimed at supporting carers and families during hospital discharge, including a comprehensive carers’ pack, a digital resource, and a new pilot project at the Carers Hub Lambeth. The group members discussed the importance of collaboration, sustainability, and language accessibility in these resources, with plans for further development and translation. The meeting also highlighted the challenges faced in hospital discharge and capacity, and the need for more integrated work with partners and other local authorities.

Matthew Mckenzie welcomed everyone to the London Hospital Discharge Toolkit group meeting. The meeting aimed to keep the momentum going on a resource that helps hospitals engage more families and carers, especially during discharge. Matthew encouraged participants to introduce themselves and share their experiences. The attendees included representatives from Tower Hamlet Carers, Barnet Carers, Sutton Carers Centre, Lewisham & Greenwich NHS Trust, Greenwich Council, Greenwich Carers Centre, St Georges University hospital trust or GESH, Lambeth Carers Hub, Bexley Carers Centre and unpaid carers. Each participant shared their roles and experiences in their respective organizations, with a focus on hospital discharge and carer support. The conversation ended with Matthew encouraging further participation and updates on the toolkit’s progress across the London hospitals in order to work with carer centres and local authorities.
Carers Hub Pilot Project Update
Rachael discussed the progress of a new pilot project at the Carers Hub Lambeth, which involves a hospital discharge lead supporting carers and promoting carer awareness. She mentioned the introduction of an additional tier of service for registered carers and the need to join forces with other GSTT and Kings College NHS trust to support carers. Rachael also expressed interest in discussing the project developments further with Matthew and others in the New Year.

Greenwich Council then presented the Greenwich Carers Pack, a comprehensive information booklet developed in co-production with unpaid carers in Greenwich. The pack includes information about carers’ rights, assessments, and support, as well as details about local community resources. Greenwich council mentioned plans to translate the pack into Nepalese and distribute physical copies to hospitals, GP surgeries, and community centers.
Carers Pack Development and Resources
Evie who chairs Greenwich Councils Carers Partnership board then discussed the development of a carers pack, which was designed to be interactive and easy to navigate. The pack covers various resources available to carers, including local and national ones, and provides bite-sized notes for carers to jot down important information. It also includes sections on employment rights, respite, legal responsibilities, financial support, home safety, and advocacy. The pack is designed to be a one-stop resource for carers, with links to all the resources mentioned. Evie also mentioned that the design team has done an excellent job, and the pack will be further developed as it goes to double pages. Matthew expressed his appreciation for the pack and requested the link to it when he runs his carer stall at the hospitals.
Digital Resource and Carer Navigation
Greenwich Council thn discussed the development of a digital resource and physical copies for a project, with plans for posters featuring QR codes for easy access. The project was well-received, with a carer and Matthew expressing their appreciation and interest in using it for their respective areas. A carer also highlighted the importance of connection and navigation for carers, noting that many learn from other carers rather than official sources. The team agreed to continue developing the project and to share it with other local authorities.
Improving Carers’ Information Pack Development
A carer expressed concerns about the lack of connection and input from various parts of the system in the development of the carers’ information pack. She highlighted the need for a more comprehensive approach, especially considering the cross-borough nature of some carers’ support. Greenwich council representive acknowledged these concerns and explained that the pack was developed by a different team, with input from Oxleas NHS trust and other organizations. She also mentioned that they are working on a more summary version and translations. The team agreed on the need for more integrated work with partners and other local authorities.
Comprehensive Carer Handbook Development Discussed
Members continued to discuss the development of a comprehensive handbook for carers. The presenters clarified that they were not planning to create a smaller, bite-sized version of the handbook, but were open to feedback suggesting such a change. The handbook will be available in various locations, including GP practices, libraries, and community centers, and can be accessed digitally via QR codes. THey also mentioned the importance of keeping the information up to date and being mindful of sustainability policies. A hospital representative expressed interest in sharing the document with other boroughs and asked about contacts within the hospital for potential distribution of the handbook. They agreed to check with colleagues about existing contacts and welcomed any additional contacts. The group encouraged others to share relevant contacts.
Consistent Information for Carers
Greenwich Council reps emphasized the importance of having consistent information spread across South East London, particularly for carers. Greenwich Carers representative praised the new greenwich council carers resource, noting its potential to be a valuable resource for carers. She also mentioned the commitment to keeping the information up-to-date, particularly on the digital portal. Evie added that they plan to translate the pack into Nepalese and other key languages for carers in the borough, and also consider developing an easy-read version. Matthew ended the conversation by noting the ease of language changes in a digital format.
St Georges Hospital NHS Trust Progress and Future Plans
Wendy from St Georges hospital who shared her team’s achievements, including virtual training sessions, bespoke staff training, and the upcoming launch of a carers’ information section on the St. George’s website. Wendy also mentioned her goal for 2025: developing a carers’ charter and survey. The team expressed their anticipation for the upcoming carers’ forum, which Matthew will be attending.

Carer Support Challenges and Progress
Tower Hamlet Carers Centre discussed the challenges and progress of their work in Tower Hamlets at royal london hospital which one of the 5 hospitals under Barts NHS Trust.
Tower Hamlet Carers centre representative is expressed her hope for having volunteers who were carers themselves to help provide the service. She also mentioned a plan to create a co-produced pack of resources for carers, which would be based at the hospital’s front desk. She highlighted the difficulty in discharge planning due to the pressures of the hospital system, which sometimes led to carers not being fully involved. Despite these challenges, Tower Hamlets Carers centre expressed optimism about the service’s progress and future plans, including the potential addition of more carer support workers. Wendy from St Georges offer her support, which I thought was very admirable.
Barnet Carers Centre update
Matthew then handed over to Mike the CEO of Barnet Carers Centre, who presented a project aimed at directing carers to the right support organization through a portal. The portal, currently under development, would direct carers to the appropriate center based on their postcode. Mike also mentioned the project’s expansion to include mental health and allied health professionals this would be the merged Mental health trusts Camden & Islington and Barnet, Enfield & Haringey who have combined into north london mental health partnership.
A carer raised a question about identifying carers during pre-assessment, to which Wendy Doyle responded that their system includes a question about whether the patient is a carer. The possibility of discussing this further in a future meeting was left open.
This concludes the short update to continue progression of the excellent legacy Debbie husting has left for London hospitals and beyond.
Welcome back to another blog post by carer activist Matthew McKenzie. I usually blog to help to educate unpaid carers on navigating health systems and strengthening their carer identity.
Today we are looking at why and how carers can escalate complaints if disatisfied about responses from health or social care services.

I have also done a video if you wish to see examples of complaints and escalations. (23 Minutes). Please click on the video below to watch.
As an unpaid carer you can learn how to navigate escalating complaints in unpaid care, from informal concerns to legal action and media attention. Empower yourself to advocate for quality care and address systemic failures effectively.
Navigating the complexities of healthcare systems can be challenging, especially for unpaid carers who dedicate themselves to looking after a loved one struggling with long-term mental or physical health issues.

Often, situations may arise where the care being provided falls short of acceptable standards, compelling carers to lodge complaints. Unfortunately, not all carers are well-informed about how to escalate these complaints effectively. This blog provides a comprehensive guide to unpaid carers on escalating complaints in various stages, from initial informal resolutions to severe legal actions.

Before delving into the stages of complaint escalation, it’s crucial to understand why raising concerns and complaints is so important. Complaints serve multiple purposes—they highlight deficiencies in the system, enforce accountability, and, most importantly, ensure that the care recipient gets the best possible treatment. Carers must recognize that it’s their right to complain if the services provided do not meet acceptable standards.

The first step in resolving any issue should ideally be informal, characterized by direct and immediate communication with the professional involved. This could be a social worker, care coordinator, or any key member of the mental health team.

Preparation is key to a successful resolution. Carers should come equipped with detailed notes, including dates and instances of lapses or failures. Bringing along the service user’s care plan can lend weight to the complaint and provide a concrete reference for the discussion. This method is most effective for minor issues such as delays in communication or minor discrepancies in the care plan.

If informal attempts do not yield satisfactory results, the next step is to submit a formal written complaint. This involves documenting all concerns, efforts made to resolve them, and any pertinent evidence.
You can also contact your local Healthwatch to feedback on services or get advice on the best way to complain.

When writing the formal complaint, ensure to:
Generally, service providers are required to acknowledge receipt of the complaint and provide a timeline for investigation, usually ranging from 20 to 40 working days, depending on the complexity of the issue.
If the issue remains unresolved, carers can seek help from PALS (Patient Advice and Liaison Service) or advocacy services. These intermediate-level services can provide guidance, represent the complainant, and even escalate the complaint within the service provider’s framework.

PALS offers confidential advice and can work as intermediaries between the carer and the care team, helping to navigate the complaints process effectively. Advocacy services can assist in drafting the complaint and ensuring that all necessary documentation is in order.
In cases of unresolved issues, escalating the complaint to regulatory bodies like the Health Service Ombudsman or Care Quality Commission (CQC) becomes necessary.

These bodies can investigate the case further, ensuring that the complaint is handled fairly. The CQC, although not handling individual complaints, can trigger inspections if there are significant failings in service provision.

This step is most appropriate for serious concerns such as poor care quality, negligence, or unsafe practices. Carers should be aware that investigations by these bodies can take considerable time.
When harm, serious malpractice, or gross negligence is involved, seeking legal advice may be the next appropriate step. This involves consulting a solicitor specializing in healthcare or mental health law.

Selecting the right solicitor involves thorough research. Often, mental health law solicitors have extensive experience dealing with such cases and can offer valuable advice on the viability of pursuing legal action
Legal action is usually reserved for extreme cases involving significant harm or death of the service user due to negligence or severe violations of rights. Legal channels can offer compensation and bring justice, albeit at a financial and emotional cost.
As a last resort, if internal and formal channels fail, bringing the issue to the public through media or social campaigns might be necessary. This becomes relevant when the issue represents a systematic failure affecting multiple service users or carers.

Carers can contact press organizations, social media channels, mental health advocates, or relevant charities, such as Mind or Rethink Mental Illness, to amplify their concerns.
Sometimes reaching out to local Members of Parliament (MPs) can also lend significant weight to a complaint, ensuring that it gets the attention it deserves. MPs can raise systemic issues within parliamentary forums, adding another layer of accountability for the service providers.

Navigating the complaint process within healthcare systems is a multi-tiered approach, designed to ensure that carers’ voices are heard at different levels of severity. Starting from informal resolutions, progressing to written complaints, and escalating to regulatory bodies or legal action, the system provides various stages for addressing concerns. If all else fails, public campaigns and media attention can serve as powerful tools to bring systemic issues to the forefront. Understanding these steps empowers carers to advocate effectively for their loved ones, ensuring that they receive the care and support they rightfully deserve.

By following this structured approach, unpaid carers can raise concerns at appropriate levels, ultimately ensuring that their voices are heard and acted upon, bringing about meaningful change in the system.
Remember complaining about a service is never that easy, full of stress and worries, but if we do not complain then how can health and social care services improve?
It is your right to complain as a carer if you are unhappy with results. Use it!!

Welcome to a brief update of my National ethnic/global community carer forum aimed at those caring for someone living with mental illness.
Here is a brief summary of October’s ethnic carer forum.
The mental health carers forum discussed updates on carer’s work stream, the launch of the carer strategy at North East London NHS FT, and an event focused on upstreaming care and black men’s mental health. The group also discussed a research project involving carers and patients, the Rethink Mental illness on involvement in the IMPACT Network, and the Patient and Carer Race Equality Framework. Lastly, the importance of representation on CQC boards, tackling health inequalities in England, and the need for continued advocacy for change were highlighted.
Mental Health Carers Forum Updates
Matthew Mckenzie, the organizer of the mental health carers forum, introduced the event and its purpose. He mentioned that the forum is a platform for carers of minority groups to learn about new initiatives and updates from researchers and NHS trusts. Matthew also introduced Asia Zaman, the Transformation Project Manager for NELFT, who shared updates about the carer’s work stream and the upcoming launch of their carer strategy. Erica Deti, the PCREF Lead for NELFT, then discussed an event focused on upstreaming care and black men’s mental health. She highlighted the event’s success in engaging the community and the importance of incorporating creativity and cultural aspects into their work. Matthew also shared pictures from the event, which some can be seen below.

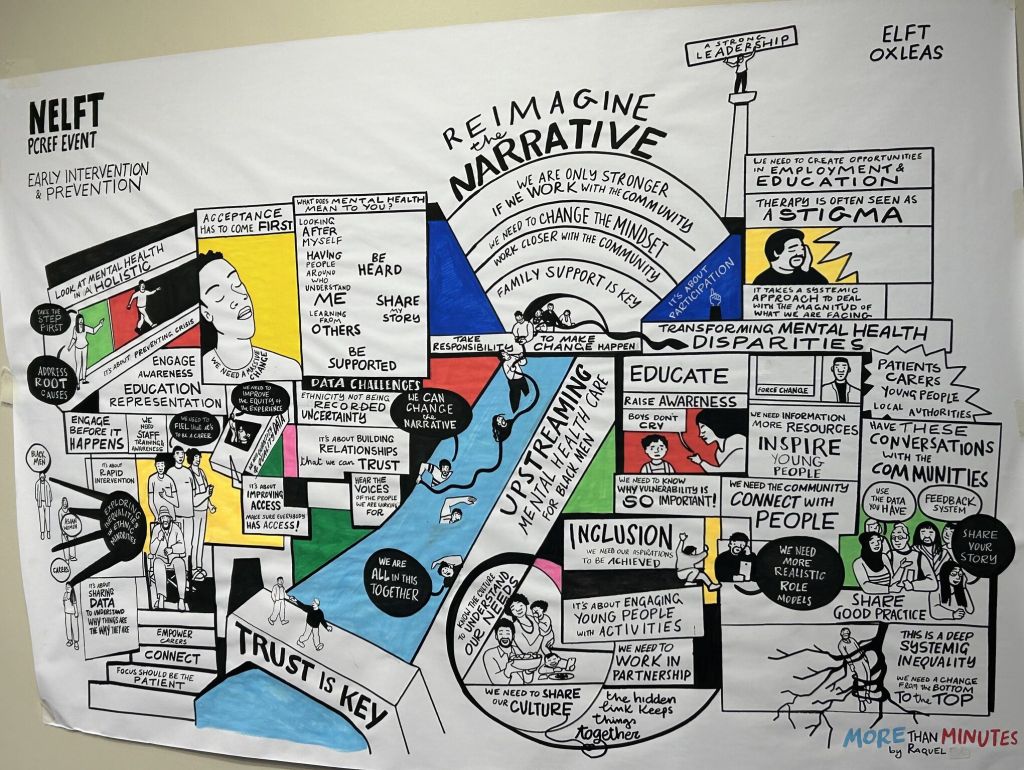









Anti-Racism Event and Carer Involvement
Matthew expressed his positive experience at the NELFT event focused on anti-racism, highlighting the multi-organizational nature of the event and the shared learning opportunities it provided. He also mentioned the launch of the Carers strategy, which he found interesting. Erica confirmed that they would be sharing the findings and learnings from the event with the group.
Marta Chmielowska at researcher at PhD Candidate in Clinical Psychology at UCL then presented her research project, which aimed to involve carers in the conversation about treatment and care in mental health services. She shared a questionnaire she developed and expressed her desire to promote it to encourage carers to participate
Marta’s Carer and Patient Project
Matthew opened the floor for any quick questions or comments for Marta, who had just presented on her project involving carers and patients. Matthew also mentioned that he would share the details of the project on his website. Marta then discussed her project, which involves a questionnaire for carers and patients to share their experiences. She mentioned that the project is online due to logistical reasons and that she has been in touch with various carer groups and charities.
For more details see poster below or email : m.chmielowska@ucl.ac.uk

Rethink Mental Illness Joins Impact Network

Ian and Ruqia from Rethink Mental Illness discussed the organization’s involvement in the Impact Network, a national organization focused on strengthening inclusion and anti-racist practice. The network, coordinated by the Universities of Birmingham and Sheffield, aims to put policy into practice and is action-oriented. The network meets four times over the next year and will decide on an action plan based on discussions and ideas. Ian and Ruqia encouraged interested individuals, including those with lived experience of severe mental illness and professionals in the mental health sector, to express their interest via email. They also mentioned that Rethink Mental Illness may have other opportunities in the future for those interested in their work.
CQC focus on Patient and Carer Race Equality Framework
Ciara and Giovanna discussed the Patient and Carer Race Equality Framework, a project they’ve been involved in since its inception. Giovanna, a senior analyst at the Care Quality Commission, explained the CQC’s role as the independent regulator of health and adult social care in England, and their oversight of almost 30,000 adult social care services. They also touched on their upcoming work, including the integration and coordination of the framework with their existing projects.

Giovanna also mentioned the publication of their annual statutory report, the State of Care report, and the legislative duties imposed on providers to register with them. The conversation ended with a discussion on the mandatory nature of the framework for all mental health trusts and NHS-funded mental health services.
Incorporating PCREF Into Regulation
In the meeting, Ciara discussed the role of the CQC incorporating the Patient and Carer Race Equality Framework (PCREF) into their regulation. They have developed interim guidance and training, and plan to use PCREF to inform their next set of guidance. They also intend to update their learning and training to support a more detailed understanding of PCREF. Ciara also mentioned the importance of including the voices of carers from ethnic minority backgrounds in their engagement and co-design of the PCREF guidance and training. The organization itself is also committed to being an anti-racist organization and plans to engage with stakeholders to add value. They are currently collecting good examples of feedback and good practice from their inspectors and mental health reviewers, and from pilot trusts. They also plan to share these examples in their monitoring the Mental Health Act Report.
For those interested, here are reports the CQC kindly presented.
Review into the operational effectiveness of the Care Quality Commission: interim report
https://www.gov.uk/government/publications/review-into-the-operational-effectiveness-of-the-care-quality-commission
Response to the interim findings of the Dash review into
CQC’s operational effectiveness
https://www.cqc.org.uk/news/stories/response-interim-findings-dash-review
Review into the operational effectiveness of the Care Quality Commission: full report
https://www.gov.uk/government/publications/review-into-the-operational-effectiveness-of-the-care-quality-commission-full-report
Professor Sir Mike Richards’ Review of CQC’s single assessment framework and its implementation
https://www.cqc.org.uk/publications/review-cqcs-single-assessment-framework-and-its-implementation
CQC responds to reviews by Dr Penny Dash and Professor Sir Mike Richards
https://www.cqc.org.uk/press-release/cqc-responds-reviews-dr-penny-dash-and-professor-sir-mike-richards
Mental Health Services Data Set
The CQC discussed the ongoing work on the mental health services data set, Version 7, which is expected to be implemented slightly later than planned to align with legislative changes. They emphasized the need for balance in managing changes to avoid disruption. A mental health trust representative asked about the new data set and review process, to which the CQC responded that they have had not heard about a new data set. A carer asked the CQC about the changes in CQC’s leadership and systems, to which the CQC confirmed significant changes and a new chief executive. Another carer asked for links to recent reports about CQC’s situation, which the CQC agreed to provide.
Representation and Board Member Experiences
Giovanna and Ciara discussed the importance of representation at their CQC board, particularly in terms of ethnicity and experiences using services. The CQC agreed to find out more about the personal backgrounds of their board members and the potential for a new board member with relevant experiences. The conversation also touched on the lack of representation of certain groups, such as clinical psychologists, in their organization. Matthew suggested that the CQC could engage with the group again in the new Year and possibly write a blog about minority mental health care.
Addressing Health Inequalities in England

Leila from The King’s Fund discussed a project focused on tackling health inequalities in England. The project, which has been ongoing since 2020, aims to identify key areas for action to be included in the anticipated 10-year health plan. Leila highlighted seven areas for action, including a cross-government strategy to address the root causes of inequality, a shift towards prevention, radically changing relationships between the NHS and communities, tackling systemic racism and discrimination, capacity building, focusing on the importance of place in this work, and prioritizing partnerships with voluntary community and social enterprise organizations.
Leila emphasized the importance of amplifying the voices of people who experience these inequalities and ensuring that these messages are heard and acted upon. The project’s findings are not new, but Leila stressed the need to continue raising awareness and advocating for change.
This concludes a short update of October’s National ethnic carers forum
Welcome back to another carer awareness blog post by Matthew McKenzie, carer activist and author. This time I want to raise awareness of involving unpaid carers when their loved one has been admitted to accute hospital care. To view an indepth version, please watch the video below (25 mins long). Unfortunately I messed up the presentation a bit.
In this blog post we discover the crucial role of families and carers in hospital care, from enhancing communication to improving patient satisfaction. Explore the benefits of family engagement and the impact on patient recovery.

When loved ones are taken into acute care in hospitals, the role of unpaid carers and family members becomes paramount. However, many carers find themselves at a loss, not knowing what to ask or how to be involved in the care process. On the other hand, healthcare professionals might not be well-equipped to engage with carers effectively. This article aims to explore the significance of carer involvement in hospital care, providing insights and guidelines for both healthcare professionals and unpaid carers.

One of the first and most crucial steps is to encourage visits from family members and unpaid carers. Emotional support from loved ones can significantly reduce the anxiety and fear of patients, contributing to their overall healing process. While this might not apply in every situation, particularly for patients who are communicative and understand why they’re in the hospital, it’s especially important for those who are severely unwell or suffering from mental health conditions.
Involvement of family members enhances communication, allowing them to share vital information about the patient’s history, preferences, and needs with healthcare providers. This is particularly beneficial for patients who may find it challenging to communicate effectively due to their condition. By integrating the carer’s perspective, healthcare professionals can make more informed decisions, ensuring a more comprehensive understanding of the patient’s situation.

Family engagement provides essential emotional support, which can motivate the patient to recover more effectively. Knowing that there’s someone rooting for them can significantly impact a patient’s willingness to adhere to treatment plans and protocols.
Carers can act as advocates for the patient, ensuring their voice is heard, especially in complex medical scenarios. This is crucial for patients who may not be able to advocate for themselves, such as the elderly or those with mental health issues.

When family members visit, they bring invaluable insights into the patient’s history and preferences, which can be instrumental in tailoring the care provided. This ensures that healthcare professionals have the most accurate and up-to-date information, thereby improving the quality of care.
Collaboration with family members in treatment decisions ensures alignment with patient values. Failing to involve carers can lead to a higher risk of readmission, as the patient might be discharged without proper support or understanding of their condition.
Emotional support from family members can significantly reduce the patient’s anxiety and foster a sense of hope, encouraging them to adhere to treatment plans and look forward to recovery.
Family involvement can also enhance treatment and discharge plans, ensuring they are more comprehensive and suited to the patient’s needs. This collaborative approach helps in creating a more effective care plan, reducing the likelihood of complications or readmission.

Healthcare providers need to ensure that family members and unpaid carers are well-informed about the patient’s condition, treatment plans, and potential discharge details. This is vital for the carer’s preparedness and ability to provide effective care post-discharge.
Hospitals should facilitate effective communication by providing resources like leaflets about available services and how to navigate the healthcare system. This not only helps in ensuring the patient’s needs are met but also empowers carers to communicate effectively with healthcare providers.
There should be advocacy resources available on-site or through referrals, helping carers navigate the complex healthcare system. This ensures that carers are not left in the dark and can effectively support their loved ones.

A holistic approach to care considers both the patient and the carer’s emotional and physical needs. While the primary focus is on the patient’s recovery, ignoring the carer’s well-being can lead to a less effective care environment.
Creating a comprehensive healing environment involves addressing the emotional distress of both patients and their families. This can lead to better overall outcomes and a more supportive atmosphere for recovery.

Establishing clear communication channels between healthcare providers and family members is essential. This ensures that information flows seamlessly and that both parties are on the same page regarding the patient’s care.
Encouraging active participation from carers in the decision-making process ensures that they are engaged and informed. This collaborative approach leads to better health outcomes for the patient.
Providing educational resources helps carers understand the patient’s condition and treatment plan better. This is crucial for ensuring that they can provide effective care post-discharge.

Involving carers in care planning and goal-setting ensures that treatment plans are aligned with patient values and that the carer is prepared for their role. This collaborative approach reduces the risk of complications and readmission.
In summary, involving family members and unpaid carers in hospital care is crucial for improving patient outcomes. By encouraging visits, enhancing communication, and providing necessary resources, healthcare providers can ensure a more holistic and effective care environment. This not only supports the patient’s recovery but also empowers carers to take on their roles confidently and effectively.

Another blog post by carer activist Matthew Mckenzie on how caregivers can engage with Integrated Care Systems to ensure their voices are heard and needs are met. A way to discover the power of feedback in improving local Health Services.
To watch the video version of my blog, click below
Integrated Care Systems (ICS) have been shaping the landscape of healthcare in the UK for several years now. These ICSs are designed to ensure that health services meet the unique needs of local communities, ICSs are evolving frameworks within the National Health Service (NHS). They aim to promote a more collaborative approach to healthcare by engaging with everyone involved in the health service delivery—including professionals, patients, and carers….yes, thats right! Unpaid carers, but how can unpaid carers get their voice heard?

Well if you are caring for someone unpaid with a long term illness, then understanding how these systems work is crucial for anyone reliant on or working within the NHS. This article delves into what ICSs are, their importance, and how carers can make their voices heard within these systems.
As noted in my video. An Integrated Care System (ICS) is essentially a model used within the UK’s NHS to better structure how health services are commissioned and provided. Before ICSs were implemented, health services were commissioned in a somewhat isolated manner, which often didn’t fully account for the comprehensive needs of the community. There were other reasons for the change to ICS, but that would be for another blog post.
At the heart of an ICS is the concept of engagement. For an ICS to be effective, it must listen to the very people who use and provide the health services. This involves unpaid or informal carers, patients, and other healthcare providers all collaborating to ensure that the healthcare services are as effective and efficient as possible
Commissioning still plays a central role within ICSs. Commissioners work to ensure that the right health services are provided, but their decisions must be informed by feedback from carers as well. This is where the role of carers becomes critical. By participating in the engagement process, carers can help shape the nature and delivery of healthcare services to better meet their needs as well as those of the patients. Carers should have a seat at the table.

One of the most effective ways to engage with an ICS is through your local Healthwatch. Healthwatch organizations are pivotal stakeholders within ICSs. They gather insights from patients, carers, and the general public to inform health service delivery.

Even if you can’t make it to meetings, there are other ways to ensure your carer voice is heard. It could be as simple as sending an email or filling out a survey provided by your local Healthwatch.
As mentioned in my video, one crucial area carers should focus on is advocating for transparency in the ICS decision-making process. Are carers and caregivers’ experiences included when tailoring health services?
Another vital strategy for making an impact in an ICS is building alliances. Networking with other carers, healthcare providers, and advocacy groups can amplify your voice.
Engage with other carers and learn from their experiences. Information sharing can be incredibly powerful.
Attending meetings and reading through reports can seem daunting, but they offer a wealth of information. One thing noted about ICSs is the amount of reports. Those reports should be held to account regarding jargon, although being relistic, there is no quick escape from Jargon.

ICSs are designed to be collaborative, ensuring that health services are well-rounded and holistic. However, this is only possible if carers, who are often the hidden backbone of healthcare provision, speak up and engage.
Carers are the crucial link between the healthcare system and the person being cared for. Without their input, ICSs may second guess the needs of the community, leading to services that do not fully meet those needs.
One of the worst outcomes for any carer is isolation. Engaging with ICSs not only helps improve healthcare services but also connects carers with a supportive network of individuals who hopefully can understand their struggles.
Beyond the immediate benefits, carer input helps create a more responsive and effective healthcare system. This leads to better outcomes for everyone involved, from the patients to the healthcare providers. Caring for someone should not always remain an isolating experience. As a carer use your experiences to ask for better support from the healthcare system.
Integrated Care Systems represent a significant step towards more inclusive and comprehensive healthcare in the UK. They aim to mesh the various elements of health service provision into a coherent whole that genuinely meets the needs of the community. Carers have an indispensable role in making this vision a reality.
By engaging with local Healthwatch, providing persistent and specific feedback, advocating for transparency, building alliances, and staying continuously informed, carers can significantly influence the effectiveness of these healthcare systems. Remember, as a carer, your insights are invaluable.
So, don’t be silent. Speak up, engage, and help improve local health services today. Together, we can achieve more adaptive and efficient healthcare systems that better serve everyone.

Welcome back from another blog post by matthew McKenzie. In today’s blog post, we’ll delve into a significant yet often overlooked initiative in the mental health sector—the Patient Care Race Equality (PCREF) Framework. Introduced by the NHS, the PCREF Framework is a pioneering approach to addressing racial inequalities in mental health services.
I have made a video (unfortunately not so short) drawing from my lived of a carer and activist. In the video I explored the core goals, benefits, challenges, and the broader implications of this framework. The video is coming from a carers pespective.
Understanding the PCREF Framework
What is the PCREF Framework?
Basically, the Patient Care Race Equality (PCREF) Framework, developed by NHS England, aims to address racial disparities within the mental health system. Data shows that racial minorities are disproportionately affected by inequalities in mental health care. The PCREF Framework seeks to improve access, experience, and outcomes for racialized communities, pushing for modernization of the mental health act and the elimination of institutional racism.
Things need to change
Mental health services have long been riddled with systemic biases and inequalities. The Mental Health Act of 1983, has aged and requires significant updates to reflect equity in care. The PCREF Framework is a part of broader efforts to reform the mental health act and address the institutional racism that has led to difficult experiences and outcomes for patients from racialized communities.

Goals of the PCREF Framework
The primary goal of the PCREF Framework is to reduce racial disparities in mental health care. This includes:
Benefits of the PCREF Framework
Targeting Inequalities
The Framework is designed to specifically target racial inequalities in mental health outcomes. For instance, racialized communities often face higher rates of severe treatments such as restraint or use of strong medications that inhibit functionality without offering therapeutic benefits. By targeting these disparities, the PCREF Framework aims to provide more equitable forms of treatment.

Improving Experiences
Another significant benefit is the enhancement of patient experiences. Historically, racialized patients have reported poorer experiences within the mental health system. By acknowledging and addressing institutional biases, the Framework seeks to transform these experiences positively.
Promoting Institutional Reform
The PCREF Framework advocates for institutional reforms to dismantle systemic barriers faced by racialized communities. This includes educating mental health professionals on cultural competencies and biases, and promoting anti-racist and anti-oppressive practices.
Enhancing Community Involvement
One of the standout features of the PCREF Framework is its focus on involving patients and carers in the decision-making process. Engaging with the communities directly affected by mental health services ensures that their voices are heard and considered in policy development and implementation.
Challenges of the PCREF Framework
As addressed in the video, there are challenges, which are listed below.

Lack of Resources and Funding
One of the most significant challenges facing the PCREF Framework is the lack of resources and funding. The NHS is already stretched thin and requires substantial investment to ensure the long-term success of this initiative. Historically, previous racial equality initiatives have failed due to insufficient financial support, and there is a risk that the PCREF Framework could face the same fate.
Risk of PCREF Being Sidelined
The PCREF Framework requires a considerable amount of commitment and resources. There is a real risk that it could be sidelined if the requisite financial and human resources are not made available. The initiative demands a comprehensive approach involving medical professionals, community workers, and continuous community engagement.
Consistent Implementation
Inconsistent implementation across different regions is another significant challenge. The success of the PCREF Framework heavily depends on effective leadership and engagement at all levels. If some NHS Trusts are more committed than others, the disparities that the framework aims to address could inadvertently be exacerbated.
Cultural Shift within the NHS takes time
The cultural shift required to fully implement the PCREF Framework is considerable. Such a shift is often slow and can be met with resistance. While the framework provides a structure for reducing racial inequalities, changing long-standing biases and practices within the NHS will require time and sustained effort.
Staff Training
To effectively implement the PCREF Framework, staff need to be adequately trained in anti-racist practices (This training should involve patients and carers) . However, current constraints such as lack of time, staff, and resources can make this a daunting task. Without proper training, the framework risks being ineffective.
Risk of Becoming a Tick-Box Exercise
One of the most critical challenges is the risk of the framework becoming a mere “tick-box” exercise. If the framework is not implemented in the spirit it was intended, it could fail to bring about meaningful change. Robust monitoring and evaluation mechanisms are essential to ensure that the framework is genuinely making a difference.
Moving Forward: Steps to Take
Community Engagement
Continuous community engagement is crucial. Mental health trusts should run engagement events and stakeholder groups to reach out to marginalized communities, understand their concerns, and incorporate their feedback into service delivery.
Tracking Progress
Regular tracking of progress and measuring the impact of the framework is vital. This involves collecting and analyzing data to assess whether racial disparities are being truly reduced. Transparency in sharing this data will help build trust and ensure accountability.
Leadership
Strong leadership is fundamental to the success of the PCREF Framework. Leaders within mental health trusts must be committed to the initiative and work towards fostering a culture of inclusivity and equity.
Education and Training
Ongoing education and training for staff on cultural competencies and anti-racist practices will help in addressing biases and promoting equitable care. As a reminder this should involve patients and carers in training programs to provide real-world perspectives and insights.
Policy Development
Ensuring that the voices of marginalized communities are heard and represented in policy development is essential. Mental health organizations must prioritize inclusivity in their policy-making processes to reflect the diverse needs of the populations they serve. The problem is things can be rushed to meet targets.
Conclusion
As I have mentioned in my video, Patient Care Race Equality (PCREF) Framework represents a significant step forward in addressing racial inequalities within the mental health system. While the benefits of this initiative are substantial, the challenges it faces are equally significant. Overcoming these challenges requires a effort from all stakeholders involved, including mental health professionals, community leaders, patients, and carers.
By fostering a culture of inclusivity, investing in resources, engaging with communities, and continually tracking progress, the PCREF Framework has the potential to bring about meaningful and lasting change. It is an ongoing journey, but with sustained commitment and collaborative effort, we can build a more equitable mental health system for all.

Welcome back to another blog post from carer activist Matthew McKenzie. I am involved in quite a few things to raise awareness of unpaid mental health carers. One of them is Carers Trusts Triangle of Care Framework.

Triangle of Care is a framework developed to improve collaboration between mental health services, service users (patients), and carers. It was created by the Carers Trust in the UK, focusing on involving carers (family members or friends who support individuals with mental health issues) in care and treatment decisions, while ensuring they receive the support and recognition they need.
We have many mental health trusts who are members of the Triangle of Care. One of them is Avon and Wiltshire Mental Health Partnership NHS Trust or AWP for short.

Avon and Wiltshire Mental Health Partnership NHS Trust (AWP) is the lead provider of healthcare for people with serious mental illness, learning disabilities and autism across Bath and North East Somerset (BaNES), Swindon and Wiltshire, and Bristol, North Somerset and South Gloucestershire.
With support from Laura Sheridan who leads on carers at Cygnet. We both attended and supported the event at the mental health partnership trust. I took the time to explore the wonderful area of Bristol. Everyone I met was welcoming and friendly.










AWP have taken up the challenge to implement the Triangle of care and listen to carers. One of the best ways to listen to carers is through engagement and celebration events.
So on Thursday 3rd of October Avon and Wiltshire Mental Health Partnership NHS Trust (AWP) ran their #LetsHearCarers event. The event was held over at Somerdale Pavilion, Keynsham.

The day started off with a welcome from Sarah Jones, Director of Nursing and Quality at AWP.
We then got to hear from Ayesha Ahmed-Mendoza on the Black2Nature campaign to enable minorty ethnic children to have better access to nature camps. Next I was impressed with the presentation from Elaine Bennett regarding experiences of deaf carers.
Then we had the panel of carers giving their experiences of involvement at the NHS trust. I personally feel involvement of carers shaping services is a powerful way of allowing carers to have their say.








After the break, we got to hear from Debbie Hustings who is the new Triangle of Care lead for Carers Trust. Debbie used to be the former NHS England carers lead for London and has a wealth of experience when it comes to unpaid carers. Debbie presented on carers rights as she presented with her carers hat on. Next there was a comedy session from Angie Betcher who is a comedian at Bristol university, she is also skilled as a poet as well as a comedy performer.

Next was Lunch and workshops to cater for the wellbeing of carers who attended.





Have lunch I was up to read out 2 poems. One of the poems you can see from Avon and Wiltshire Mental Health Partnership NHS Trust’s video of the carer event below.
After more performances and networking with carers, I headed home. I would like to thank Avon and Whiltshire for the excellent event they put on for the community. Everything was planned brilliantly and I did not hear any grumbling from carers. I look forward to more events in future.
