By Matthew McKenzie – Chair of the Carers Hospital Discharge group

Hospital discharge remains one of the most critical and stressful moments for unpaid carers, patients and healthcare professionals alike. During the recent Carers Hospital Discharge Group meeting held in May 2026, professionals, carers, NHS leaders, hospital representatives and community organisations came together to discuss major developments affecting carers across London and beyond.
The Carers Hospital Discharge meeting runs every 2 months and for the month of May we discussed improving hospital discharge processes, strengthening carer identification, digital inclusion, community support and the growing role of technology in healthcare planning.
The blog update is for those unable to attend, here is a summary of the key discussions, presentations, questions and responses shared during the session.
Universal Care Plan Expansion Through the NHS App

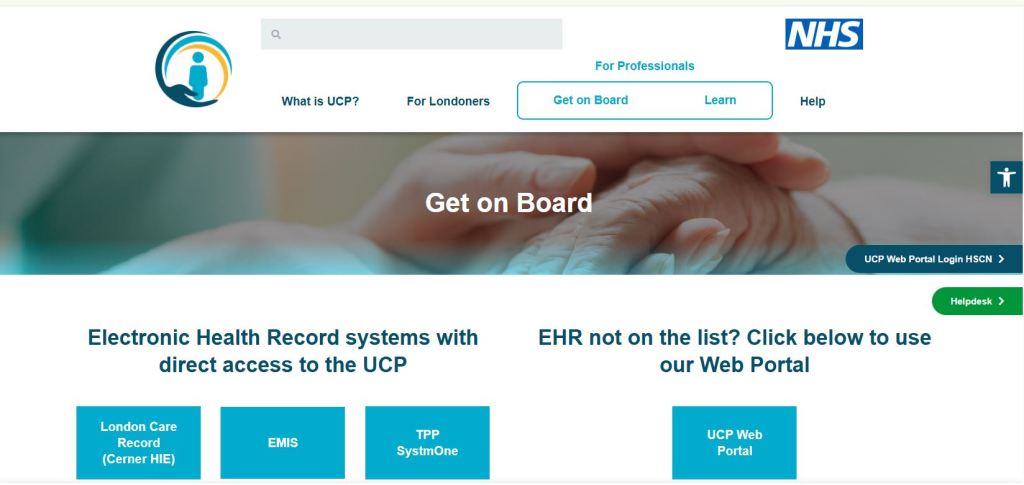
One of the biggest updates came from NHS England, who shared exciting news about the expansion of the Universal Care Plan (UCP).
The new development allows patients and members of the public to begin creating their own Universal Care Plans directly through the NHS App. Previously, only clinicians could initiate many aspects of these plans.
NHS England explained that editable sections now include areas such as:
- “What matters to me”
- Communication preferences
- Care and contingency plans
- Personal support needs
Clinical sections, however, remain under healthcare professional control.
Updates described the project as a major milestone after years of discussion about allowing people greater control over their own care information.
Question from attendee:
“Will carers be able to input on behalf of their cared-for person?”
response from presenter:
At present, carers cannot directly complete plans on behalf of another person due to safeguarding and proxy access concerns. However, carers can still complete their own care contingency plans within the system.
It was explained that this means if a carer suddenly becomes unable to provide care, emergency services and healthcare providers would be alerted that a contingency plan exists.
They also noted that community organisations could potentially support individuals with completing plans, provided appropriate governance and data security arrangements are in place.
The discussion highlighted both the opportunities and challenges of balancing digital access with safeguarding responsibilities
*****
For more developments on the Universal Care PLan, I have provided the link below of the recent Webinar
UCP Webinar: Supporting Patient Editable Access to the Universal Care Plan – Guidance for Professionals (May 2026)
https://vimeo.com/1190395114/37af950076?share=copy&fl=sv&fe=ci
New Research on Social Networks and Healthcare Support
Matthew McKenzie introduced an emerging research project led by Queen Mary University of London alongside several major universities including Harvard, Oxford and Warwick.

The project aims to explore how patients’ social support networks influence health outcomes, hospital admissions and long-term wellbeing.
Researchers are developing tools to map patients’ support systems, including:
- Family carers
- Friends
- Peer groups
- Community support
- Online social networks
The project seeks to better understand how strong support systems can improve self-management and reduce avoidable hospital admissions.
Matthew explained that researchers are particularly interested in understanding:
- Whether support network mapping would feel helpful or intrusive
- How carers should be recognised within healthcare systems
- How cultural differences affect support networks
- What safeguards around privacy and consent are needed
The proposal sparked interest among attendees because it reflects a wider NHS shift toward community-based care and prevention.
NHS England connected the project to wider work around “family group conferencing,” where whole-family approaches are used to plan care and support more collaboratively.
NHS England’s Urgent and Emergency Care Strategy 2025/26
A major section of the meeting focused on NHS England’s emerging Urgent and Emergency Care (UEC) Strategy.
Matthew presented some notes on NHS England UEC outlining plans to:
- Reduce avoidable hospital admissions
- Deliver more care within communities
- Expand digital healthcare access
- Improve hospital discharge pathways
- Strengthen operational efficiency
Key proposals included:
- AI-enabled triage systems
- NHS App navigation tools
- Digitally coordinated urgent care
- Expanded community-based treatment
- Greater use of early intervention models
However, the discussion quickly moved toward the potential risks associated with rapid digital transformation.
Participants concerns:
Representatives covering Hospitals, raised important concerns about how discharge pressures could negatively affect carers.:
“If somebody urgently needs that hospital bed, the pressure becomes getting people discharged quickly. That may not always leave enough time to identify carers properly.”
They stressed that carer identification should happen throughout the patient journey not only during discharge.
They highlighted opportunities for identification during:
- Outpatient appointments
- Pre-assessment clinics
- Routine hospital interactions
Concerns About Digital Poverty
Another major concern involved digital exclusion.
Participants warned that:
- Older people
- People with dementia
- Individuals without smartphones
- People facing poverty
- Non-English speakers
- Neurodivergent individuals
could all struggle if urgent care becomes too dependent on digital systems.
It was mentioned that meeting carers who still rely entirely on phone calls rather than online platforms and stressed the need for alternative accessible routes into care.
Others agreed and referenced an Equality Impact Assessment linked to the NHS 10-Year Plan, which explores risks around digital inequality and vulnerable groups being left behind.
Equalities Impact Assessment – 10 Year Health Plan for England
https://www.gov.uk/government/publications/equalities-impact-assessment-10-year-health-plan-for-england/equalities-impact-assessment-10-year-health-plan-for-england
You can find out more about the UEC below
https://www.england.nhs.uk/publication/urgent-and-emergency-care-plan-2025-26
Carers Week Preparations Across London and Beyond

Many organisations shared updates on activities planned for Carers Week 2026
NHS England
NHS England Carers Week 2026 – ‘Building Carer Friendly Communities’
https://www.events.england.nhs.uk/nhs-england-carers-week-2026-building-carer-friendly-communities
Kingston Carers Network
KCNshared plans for:
- Benefits advice sessions
- Afternoon tea events
- Mental health awareness activities
- Community picnics
- Outreach work with carers across Kingston
A major highlight will be the attendance of Sir Ed Davey, who is himself a well-known advocate for unpaid carers due to his own lived experience caring for family members. His involvement is expected to help raise awareness of the challenges carers face daily.
KCN also spoke about Kingston Carers Network’s ongoing efforts to strengthen links with Kingston Hospital. The organisation already receives referrals through the hospital’s carers liaison department, helping unpaid carers access emotional support, information and practical guidance following hospital admissions or discharge.
However, KCN is now trying to expand its presence inside the hospital itself through more direct face-to-face outreach work. Plans are being discussed to establish regular information stands within hospital settings so carers can receive support earlier and more proactively.
KCN explained that while these conversations are progressing, coordinating regular in-hospital outreach remains challenging due to logistical pressures and scheduling issues. Despite this, the organisation continues to work closely with hospital teams to improve visibility and engagement with carers.
Beyond hospital settings, Kingston Carers Network continues to deliver several outreach programmes throughout the borough. Staff regularly attend local groups, community spaces and events to identify carers who may not realise support is available to them.
North Central London Carers Support Project
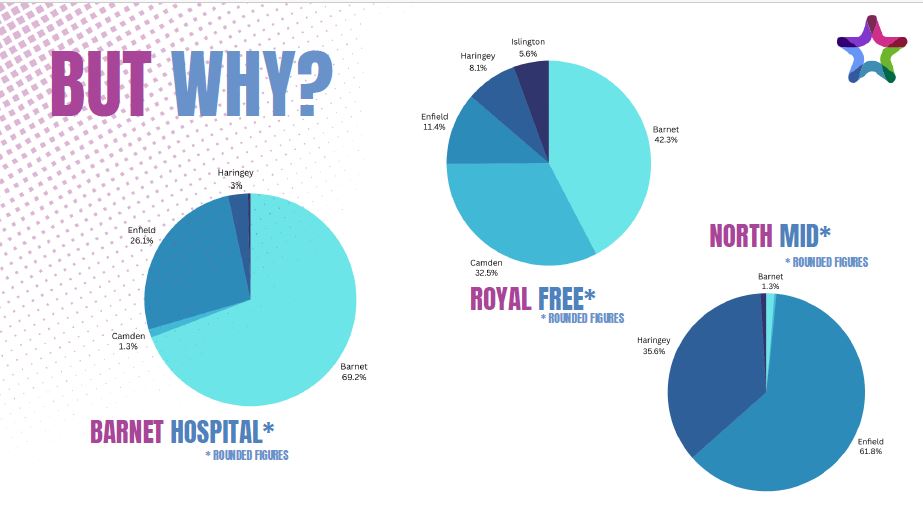
Eleanor updated the group on work taking place across:
- Barnet
- Camden
- Enfield
- Haringey
- Islington
The project works in partnership with multiple NHS trusts and carers organisations across North Central London with the aim of creating a more consistent and coordinated approach to identifying and supporting unpaid carers.
At the centre of the programme is the development of a standard operating procedure for carers within hospitals and healthcare settings. The goal is to ensure carers are recognised earlier, referred more efficiently and supported more consistently regardless of which hospital or borough they engage with.
One of the project’s biggest developments has been the creation of a dedicated carers referral website. Eleanor explained that the system is designed to simplify the referral process for healthcare professionals. When a referral is submitted through the portal, the system automatically directs the carer to the appropriate local carers organisation based on their postcode.
The intention is to remove confusion for hospital staff while helping carers access support much faster.
Eleanor described the project as an effort to make support pathways:
- Easier for professionals to navigate
- More accessible for carers
- Better integrated across borough boundaries
- Less dependent on individual staff knowledge
A major focus of the project continues to be embedding carer awareness into everyday hospital practice.
Carer Awareness Training Expanding Across Hospitals
The team has made significant progress with carer awareness training sessions delivered across several NHS trusts.
Regular drop-in training sessions are now taking place with:
- The Whittington Trust
- The Royal Free
- North London Mental Health Trust services
Eleanor shared that attendance at some sessions has now exceeded 40 healthcare staff members, which she described as a major success.
The training focuses on:
- Identifying unpaid carers earlier
- Understanding carers’ rights and needs
- Improving referral pathways
- Increasing staff confidence when supporting carers
- Embedding carer recognition into routine clinical practice
Importantly, the project measures the effectiveness of these sessions using confidence ratings before and after training. Eleanor reported that most staff attending show at least a one- or two-level increase in confidence around identifying and supporting carers after participating.
North Central London’s Focus on Carers Week and Community Engagement
Preparations for Carers Week are also a major priority for the project.
The team plans to host information stalls and awareness events at several hospitals including:
- The Whittington Hospital
- University College London Hospital (UCLH)
- Barnet Hospital
These events aim to:
- Raise awareness of unpaid carers
- Promote available support services
- Encourage hospital staff to make referrals
- Help carers connect with local organisations
Lewisham Council Developments
Updates from Lewisham was on the ongoing work taking place across Lewisham to improve support for unpaid carers, particularly through closer collaboration between hospitals, carers organisations and local commissioners.
A major development has been Lewisham Hospital’s involvement in the South East London pilot programme focused on creating a standard operating procedure for carers across NHS trusts. The pilot aims to improve consistency in how carers are identified, supported and referred within hospital settings.
It was explained that Lewisham Hospital has been working closely with Imago, the borough’s commissioned carers support provider, to strengthen partnerships with hospital nursing teams and improve awareness of carers across wards and services.
Particular emphasis is now being placed on:
- Increasing carer awareness training
- Improving communication between services
- Embedding carer identification into routine hospital practice
- Strengthening links between healthcare and community support
Inspired by discussions during the meeting, it was also highlighted plans to explore integrating carer identification into regular auditing and review processes within hospital settings similar to initiatives already underway in other trusts.
Redesigning Lewisham’s Future Carers Service
One of the most significant updates involved the redesign of Lewisham’s carers support service model.
They shared that the current commissioned contract for carers services is due to end in January 2027, and work is already underway to shape the next phase of support provision.
Importantly, unpaid carers themselves are playing a central role in developing the new model.
A series of co-production sessions has been held with carers across the borough to ensure their lived experiences directly influence future service design. These discussions are helping shape priorities around:
- Access to support
- Communication with carers
- Outreach and identification
- Emotional wellbeing services
- Practical support needs
- Hospital discharge experiences
The borough hopes to move into procurement for the redesigned service later this year.
Carers Hub Lambeth
Carers Hub Lambeth shared an update on the organisation’s ongoing work supporting unpaid carers across King’s College Hospital and Guy’s and St Thomas’ NHS Foundation Trusts.
Although the current hospital carers project funding has been extended for an additional six months, Jen explained that the programme is now approaching its final phase, with funding currently due to end in September 2026.
As a result, the team’s main focus is now on ensuring hospitals become as self-sufficient as possible in identifying and supporting carers once the dedicated project ends.
Expanding Carer Awareness Training
A major priority for Lambeth Carers Hub is expanding carer awareness training for healthcare professionals.
It was explained that the organisation has:
- Increased training sessions from once to twice monthly
- Begun arranging bespoke sessions with individual hospital teams
- Expanded engagement with primary care networks
- Updated training materials to address barriers to carer identification
The training aims to help healthcare staff:
- Recognise unpaid carers earlier
- Understand carers’ support needs
- Improve referral pathways
- Build confidence in conversations with carers
- Embed carers into routine healthcare practice
Carers Hub Lambeth acknowledged that while training sessions often generate an immediate increase in referrals, maintaining long-term momentum remains challenging.
It was mentioned that a familiar pattern where professionals attend training, referrals increase temporarily, and then gradually reduce again as competing clinical pressures take over.
Because of this, the organisation is now trying to better understand:
- Why carers continue to be missed
- What barriers staff face in identifying carers
- How carer awareness can become part of everyday practice rather than an additional task
This reflects a wider challenge discussed throughout the meeting — ensuring carer support becomes embedded within healthcare systems rather than dependent on individual staff enthusiasm.
Embedding Carer Recognition Into Everyday Hospital Practice
One of the most practical discussions came from GESH update on integrating carers into routine hospital auditing processes.
St George’s and Epsom and St Helier Hospitals are now:
- Adding carer identification questions into ward audits
- Including carers within routine quality checks
- Training volunteers to identify carers on wards
- Embedding carers into “business as usual” practice
Wendy also spoke extensively about the NHS “Reasonable Adjustments Digital Flag,” a major NHS initiative designed to ensure patients’ accessibility needs are recognised across services.
The system aims to help hospitals and GP services better identify:
- Communication needs
- Disabilities
- Neurodivergence
- Mental health conditions
- Carer-related support needs
The long-term goal is for healthcare systems to automatically recognise and share reasonable adjustment requirements across services.
Final Reflections
The meeting demonstrated both optimism and concern about the future direction of health and social care.
There was strong agreement that:
- Community-based care is necessary
- Earlier intervention can prevent hospital admissions
- Carers must be identified earlier
- Digital systems offer opportunities
However, participants repeatedly stressed that healthcare transformation must not leave vulnerable people behind.
Carers remain central to safe discharge, patient wellbeing and long-term community support. As NHS services increasingly move toward digital and community-led models, ensuring carers are recognised, supported and included will remain critical.
The next Carers Hospital Discharge Group meeting is expected to take place in July 2026.