By Matthew McKenzie (Chair)
I chaired our March hospital discharge network meeting with a real sense of momentum building across the system. What continues to strike me is the mix of voices in the room, commissioners, carers centres, hospital representatives, and grassroots advocates all trying to tackle the same persistent issue: how we properly involve and support unpaid carers during and after hospital discharge.
As someone with lived experience, particularly in mental health and complex care, I always come back to one key question:
Are carers being treated as partners, or are they still being treated as visitors?
This meeting gave us a very honest answer progress is happening, but there is still a long way to go.
Key Presentation: Derbyshire HConnect Project
Emma’s presentation was, for me, an important part of the meeting not because it introduced something completely new, but because it clearly articulated what many carers have been saying for years, and then actually did something about it.

What stood out immediately was that this wasn’t a project designed in isolation. It was built directly from carer voice and lived experience. The starting point wasn’t “how do we improve discharge?” it was “what are carers actually experiencing right now?”
And what carers described was difficult to hear, but not surprising.
Carers spoke about not being recognised at all. Some said no one had even asked if they were a carer. Others described situations where their knowledge of the person they care for was ignored, even when it was critical. One example that stayed with me was a carer describing their loved one being discharged in the middle of winter, late at night, without proper clothing or preparation.
There was a consistent feeling that once someone enters hospital, the carer’s role is almost paused or worse, dismissed entirely.
What the HConnect project does differently is acknowledge that this isn’t just a communication issue it’s a system and culture issue.
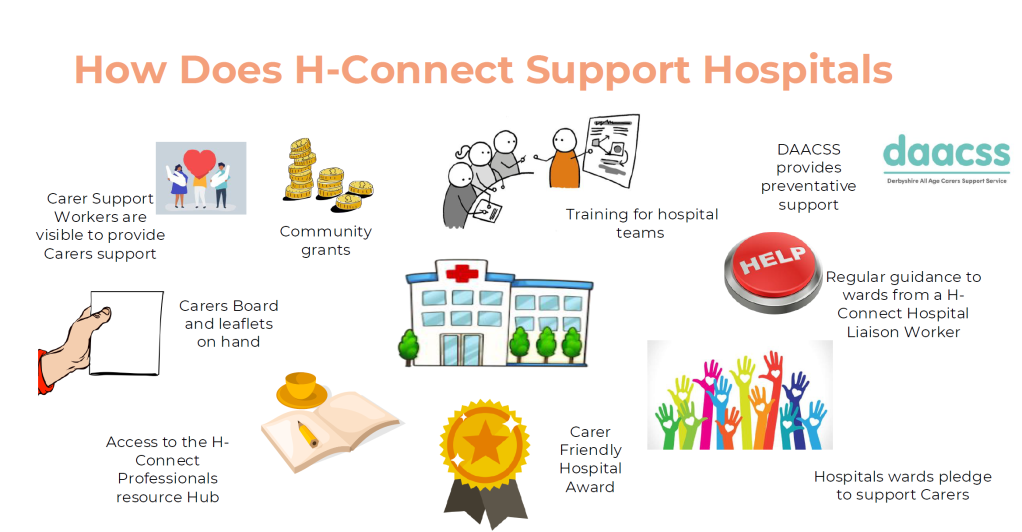
Instead of relying on one intervention, the model works across multiple layers of the hospital system. It introduces dedicated hospital liaison workers who build relationships with wards, while also ensuring carers themselves are visible and supported directly on-site. At the same time, it invests in staff through training, guidance, and practical tools so that engaging carers becomes part of everyday practice rather than an optional extra.
What I found particularly important is that the project doesn’t assume staff are unwilling—it recognises that many staff simply lack the confidence, knowledge, or structure to engage carers properly. In fact, the findings showed that many hospital teams had never received any formal carer awareness training and were often unaware that carers even have a legal right to be involved in discharge planning.
The research element of the project adds another layer of depth. Through interviews with carers, several consistent themes emerged.
Carers described feeling invisible—treated as visitors rather than partners in care. They talked about their expertise being dismissed, even when they knew the patient best. Communication was often unclear or inconsistent, and discharge frequently felt rushed, with little notice or preparation. In many cases, carers ended up acting as the safety net catching mistakes, coordinating care, and managing complex needs on their own once the person returned home.
What struck me most is that these issues aren’t just isolated incidents they are patterns.
But importantly, the presentation didn’t just focus on what’s going wrong. It also highlighted what good looks like. In situations where carers were listened to, involved early, and treated as equal partners, the entire experience changed for both the carer and the patient. The challenge now is making that level of practice consistent, not exceptional.

The project is already showing tangible impact. There has been a noticeable increase in carers being identified within hospital settings, more referrals coming directly from health professionals, and hundreds of carers receiving support through the programme.
For me, the biggest takeaway from this presentation is this:
This isn’t about adding more services it’s about changing behaviour across the system.
The HConnect model recognises that for carers to be properly involved, three things need to be in place: staff need the capability to identify carers, the opportunity within the system to engage them, and the motivation to see this as a core part of care. Without all three, change simply won’t stick.
And that’s why this work matters. Because until carers are consistently seen, heard, and included, we will continue to see the same issues repeating no matter how many initiatives we introduce.
Lewisham Commissioner Update
From Lewisham’s commissioning side, there were some strong practical developments.

A key initiative is the rollout of a carer welcome pack, designed to be:
- Clearly visible in hospital settings
- Easily accessible to carers at the point of need
This is being strengthened through:
- Increased collaboration with hospital staff
- Plans to expand distribution across wards
From Lewisham, we also received a really significant update around system-level change, particularly the development of a Standard Operating Procedure (SOP) for engaging unpaid carers in hospital settings.
This work has been led across South East London ICB, with an external partner supporting the design. The aim of the SOP is to provide:
- Clear guidance to hospital wards
- Practical prompts and questions for staff
- A consistent approach to identifying and engaging carers during hospital stays
What stood out to me is that this isn’t just a document, it’s designed to change behaviour on the ground. It focuses on something simple but powerful:
how staff start conversations with carers and recognise the people already supporting patients.
In Lewisham, University Hospital Lewisham was selected as one of the pilot sites, with two wards testing the approach. The next stage is particularly important:
- The SOP is being embedded into Trust templates
- It is due to be presented to the Trust board for formal approval
- There are plans to roll this out across Lewisham and Greenwich NHS Trust, including Queen Elizabeth Hospital (Woolwich)
What I found especially encouraging is that carers have been involved throughout:
- Input gathered through workshops
- Further feedback taken to the Lewisham Council’s Open Carers Forum
- Ongoing opportunity for boroughs to adapt the SOP to local needs
Alongside this, Lewisham is continuing practical work on the ground:
- Strengthening links between commissioned carers services and hospital staff
- Expanding visibility through carer welcome packs and information points within the hospital
For me, this is one of the most important developments discussed in the meeting. If implemented properly, a shared SOP like this has the potential to:
- Reduce inconsistency across wards
- Embed carer identification into everyday practice
- Move us closer to a system where carers are routinely recognised—not accidentally discovered
Hospital Update: Lewisham & Greenwich NHS Trust
A really important contribution came from the patient experience perspective at Lewisham and Greenwich NHS Trust, which covers University Hospital Lewisham and Queen Elizabeth Hospital (Woolwich).
From the Trust side, there was clear recognition that:
- The work carers are doing is valuable and essential to patient outcomes
- There is a need to improve physical visibility of carer support within hospital settings
- Space and infrastructure need to better support engagement (for example, identifying a permanent location for carer engagement and resources)
There was also a willingness to:
- Explore how carer-led engagement (including my own involvement) can be better embedded within the hospital environment
- Strengthen links between patient experience teams and carers organisations
From my perspective, this was a positive and practical discussion. Too often we talk about engagement in theory—but here we were talking about where the table actually goes on the ward, and that level of detail matters.
Because if carers can’t see you, they can’t access you.
Greenwich (Commissioning & Mental Health)
Greenwich colleagues spoke about their broader system approach, particularly within mental health.
Their focus includes:
- Identifying gaps in carer support across services
- Embedding carers within commissioning priorities
- Understanding what carers themselves want from local systems
They also posed an important question to the group:
What should local authorities prioritise for carers?
My answer was straightforward:
We need clear leadership and accountability, a named person or role responsible for carers across the system.
Without that, good work risks becoming fragmented.
Lambeth Carers Hub (King’s College Hospital & St Thomas’ Hospital)
Lambeth shared a detailed and honest update regarding their work across King’s College Hospital and Guys and St Thomas Hospital
Key points included:
- Their hospital discharge project is continuing, but with reduced capacity due to funding constraints
- They have secured a short-term extension, allowing work to continue until September
- A major focus is now embedding carer awareness training into staff induction processes
Importantly, they raised a systemic issue:
- The need to hold commissioned care agencies accountable, particularly when carers report poor-quality care after discharge
This is critical. Discharge doesn’t end at the hospital door—if the care package fails, the whole system fails.
Southwark Council Update
From Southwark, we heard about work being done at a system level, particularly linked to:
- Development of discharge information resources across South East London
- Collaboration across boroughs and NHS partners
The intention is for these resources to be:
- Widely accessible and adaptable
- Used across multiple organisations, rather than siloed locally
Given the proximity to major hospitals like King’s College Hospital and GSTT hosptal, this kind of coordinated approach is essential.
City & Hackney Carers Centre (Homerton Hospital)
A more concerning update came from City & Hackney, particularly regarding work linked to Homerton Hospital.
They reported:
- The loss of a hospital discharge worker role
- A significant drop in referrals to the carers centre as a result
- Reduced presence within the hospital environment
This clearly demonstrates something we often say but don’t always quantify:
When you remove dedicated roles, you remove outcomes.
The worker’s presence had been directly contributing to engagement and referrals. Without that, carers are once again at risk of being missed.
Richmond Carers Centre (Kingston Hospital)
Updates from Richmond Carers Centre highlighted both strong engagement and opportunities to build further.
Positives:
- Strong referral pathways coming through from Kingston Hospital, particularly linked to discharge activity
- Ongoing professional awareness work, helping improve understanding of carers across services
There is a clear foundation here, with established relationships already supporting carers into services. The opportunity now is to build on that by increasing visibility and strengthening in-hospital engagement further.
Richmond Borough Mind (Springfield Hospital – SWLSTG)
From Richmond Borough Mind, the focus was more specifically on their work within South West London and St George’s Mental Health Trust (SWLSTG), particularly at Springfield Hospital.
Key challenges highlighted:
- Difficulty accessing wards within Springfield Hospital, limiting direct engagement with carers
- Limited contact with carers when based in general hospital areas rather than embedded on wards
- Ongoing challenge in identifying where carers are most visible and reachable within mental health settings
What came through strongly is that, despite proactive efforts such as setting up stands and being present on-site, footfall from carers remains low unless services are embedded directly into ward environments.
This reinforces a key point for me:
In mental health settings especially, access is everything—if you’re not where carers are, you simply won’t reach them.
Bexley Carers (Post-Discharge & Reablement Focus)
Bexley brought an important perspective that often gets overlooked what happens after discharge.
Their work is focusing on:
- Supporting carers once reablement packages end
- Recognising that carers often deprioritise themselves during discharge, only to struggle later
- Increasing concern around safeguarding and mental health, particularly in dementia care
This is where we need to shift thinking:
Discharge is not the endpoint—it’s the start of a new phase of care.
Cross-Cutting Reflections
Across all updates, several consistent themes emerged:
- Inconsistent carer identification across wards and trusts
- Funding fragility, with projects often short-term
- Need for embedded training, not optional sessions
- Importance of visibility within hospital environments
- Gaps in post-discharge support, especially after reablement
My Closing Thoughts
Chairing this meeting, I was struck by both the progress and the gaps.
There is innovation happening in Derbyshire, in Lambeth, in Lewisham, across South East London. But it’s uneven. And carers feel that inconsistency every day.
For me, the priority remains clear:
- Identify carers early
- Involve them properly
- Support them beyond discharge
Because when we get that right, everything else improves—outcomes, safety, and experience.
And until we get that right consistently, we still have work to do.